
Call now for a confidential consultation with our Patient Representative • Atlanta & Beverly Hills 678-573-6965
Vesicovaginal Fistula Repair Case Study #5
Successful Laparoscopic Fistula Repair Following Two Failed Vaginal Attempts
Fistula Symptoms: Continuous urine loss from the vagina
Initial Cause of Vesicovaginal Fistula: Complication of a laparoscopic assisted vaginal hysterectomy (LAVH)
Failed Attempt to Repair Fistula: Two failed Latzko procedures - vaginal approach to VVF repair (as opposed to Miklos and Moore's laparoscopic approach)
This patient is a 35-year-old female who developed a VVF after her laparoscopic assisted vaginal hysterectomy (LAVH) performed on November 16, 2010. She claims that she began having continuous urinary leakage in February 2011 and her gynecologist referred her to the university in their state.
A urogynecologist at the university saw the patient and performed a transvaginal approach to VVF repair (known as a Latzko procedure) in May 2011. The surgery failed and the patient had a second procedure by the same urogynecologist in July 2011. Unfortunately the procedure failed. The patient commented “ I know my urogynecologist did his best but it just didn’t work and after two failed Latzko procedures he recommended that I see Dr. Miklos & Moore in Atlanta, GA. “
Dr. Miklos's comment: “All surgeons have failures and her urogynecologist did his best however he just didn’t have the skill to attempt the procedure laparoscopically,” and thus he sent the patient to Atlanta.
Drs. Miklos & Moore saw the patient on September 15, 2011 and subsequently performed surgery in October 2011. The surgery was completed in approximately in 90 minutes. After insertion of the stent Dr. Miklos & Moore performed a laparoscopy (Photo 1) and dissected between the bladder and the vagina to identify the actual fistula.
Photo 1
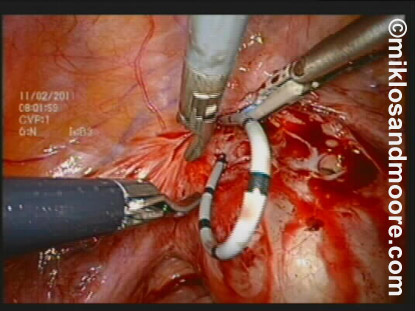
Photo 2
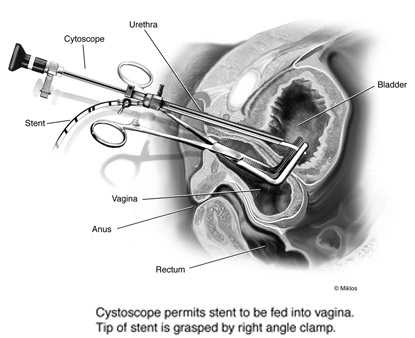
Photo 2b
The stent was divided and stent was utilized for traction and separation of the bladder and the vagina. (Photo 3).
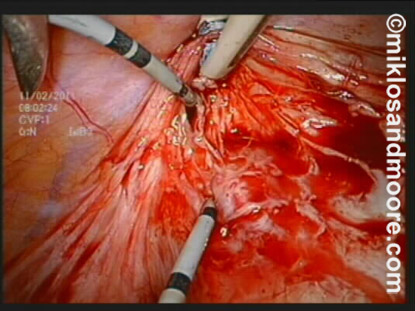
Photo 3
Further dissection was necessary to separate the bladder from the vagina (photos 4 & 5).
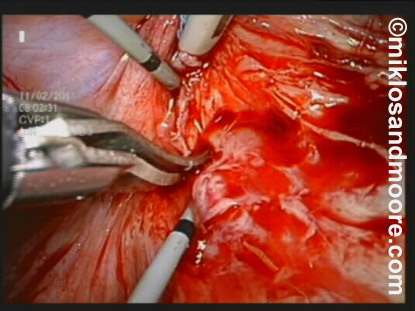
Photo 4
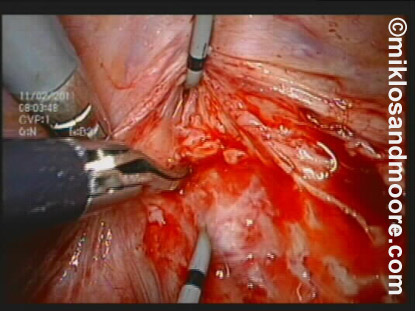
Photo 5
The bladder hole was made larger as the surgeons need to freshen up or make raw the edges of the hole in the bladder so it will heal better (Photo 6).
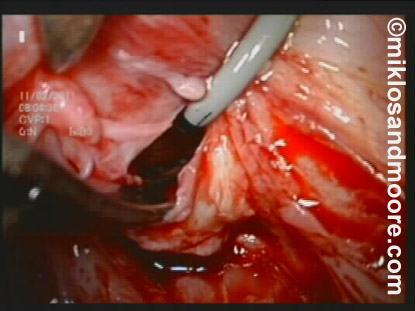
Photo 6
The bladder was closed with 2 layers of sutures (Photo 7).
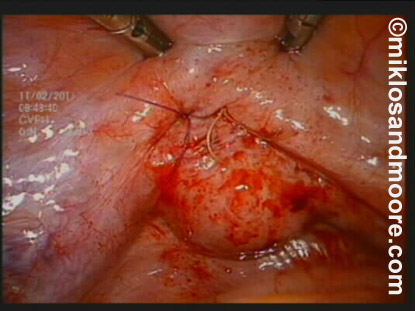
Photo 7
A cystoscopy (i.e. looking inside of the bladder) immediately after surgery revealed a perfect closure (photo 8).
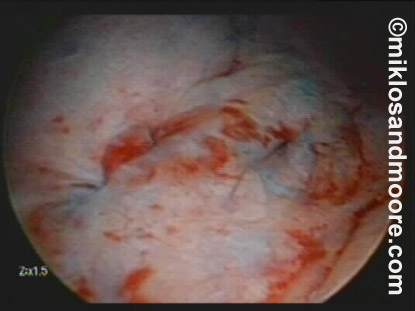
Photo 8
The next photo reveals the view from inside of the patient i.e. the laparoscopic view. Here we have a full bladder, which is testing the integrity of the newly repaired fistula. There is no leakage noted. (Photo 9)
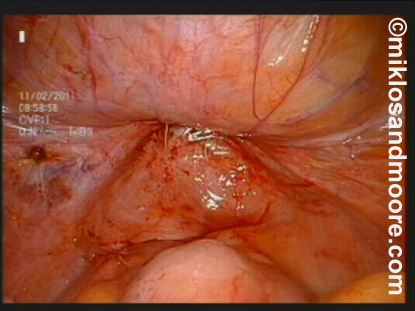
Photo 9
The patient spent one day in the hospital and then was discharged to a hotel for 2 days and the patient subsequently went home. The patient had her catheters removed 14 days after surgery and was seen 6 weeks after her surgery. A cystoscopy was performed and the VVF was declared cured by the patient, her husband and Dr Miklos.



